Index
ProLAM – Model-based optimization of the Liquid Additive Manufacturing (LAM) process

Silicone components are widely used both in industry and in medical technology. The outstanding material properties, such as high crack elongation, temperature resistance or chemical resistance, are largely responsible for this. Particularly in the field of medical technology, patient-specific solutions are also in demand, so that complex additive manufacturing systems for silicone components are also required in combination. These processes are young and difficult to control, since an irreversibly chemically reactive mixture is processed. However, advantages over indirect additive processes, casting into printed molds, exist in both complexity and cost advantages.
The research project deals with the Liquid Additive Manufacturing (LAM) process, through which complex silicone components can be directly additively manufactured. Within the process, two starting components are mixed to form an uncured silicone rubber. The rubber is then applied in web form to a build platform, where it crosslinks additively. The speed of crosslinking is influenced by the thermal energy applied.
The complex process is to be analyzed and modeled within the research project. Subsequently, the setting of process parameters can be automated and adapted to the component, which reduces the manual preparation time and prevents misprints.
Mobile, haptic scanning method for optimised detection of tissue properties in orthopaedic technology
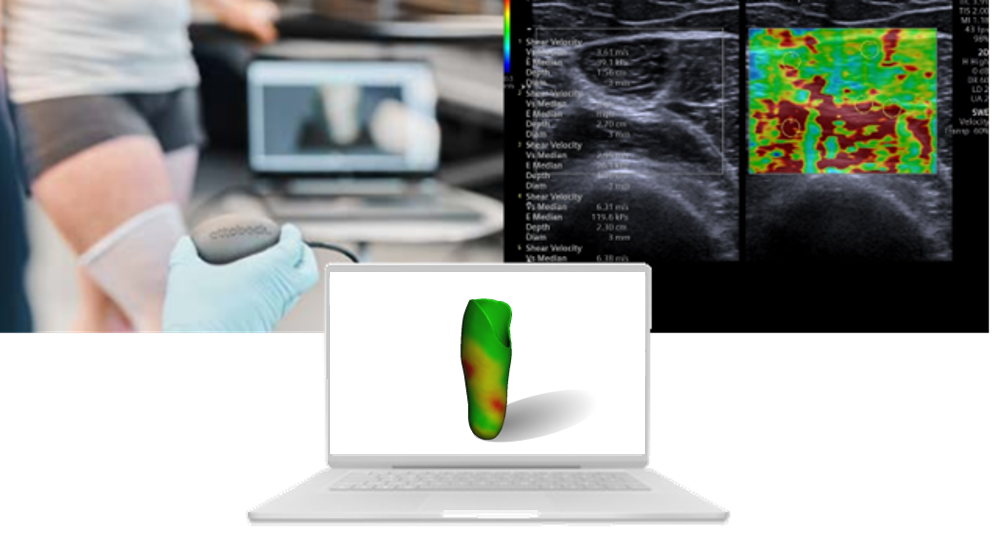
The prosthetic fitting is currently a manual procedure based on the skills and knowledge of the orthopaedic technician. Based on the manually recorded tissue structure, a plaster cast is physically modelled to create the basis for the socket geometry. Due to the subjective recording of the tissue condition, repeated adjustments of the socket, the crucial interface between the body and the prosthesis, may be necessary or incorrect fittings may occur. In addition to an inconsistent standard of care, the documentation of therapy is hampered by a lack of quantifiable data and prevents the continuous exchange of data in this interdisciplinary field between surgeons, orthopaedic technicians and therapists.
In the “HapticScan” project, the quantifiable recording of tissue data is therefore fused with data from a surface scan in order to create a holistic information basis for fitting and also to enable small companies to provide prosthetic fitting, for example, via contract manufacturing on the basis of this data basis.
The new haptic scanning system developed in the project is intended to quantify and digitally record the palpation (examination by palpation) previously carried out manually by the orthopaedic technician. For this purpose, the sensor data of an ultrasound-based measuring method will be fused with exact localisation data to enable integration into surface scanning systems available on the market
